By Phil McLachlan
All first responders in the Fernie area are now equipped to take on a potential opioid crisis.
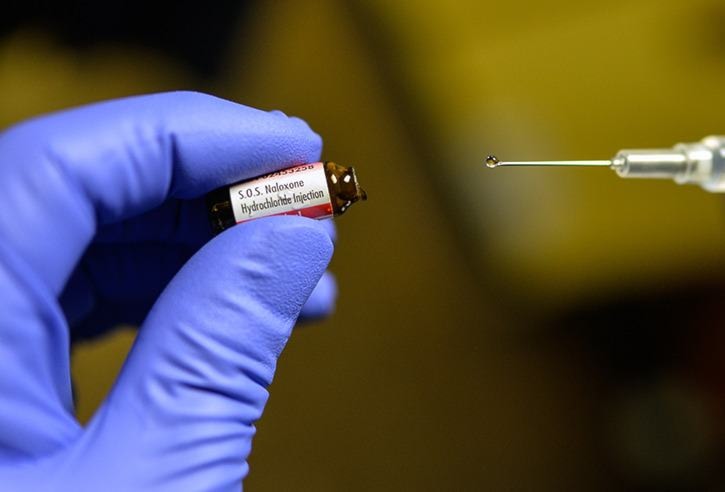
Fernie Fire and Rescue were the last group in the area to become trained in opioid overdose situations by BC Emergency Health Services. The main area of focus for training was on Naloxone, the antidote for opioid overdoses.
Unable to give any numbers at this time, Elk Valley RCMP Corporal Bob Wright did state that, “We have responded to Fentanyl drug use in the Elk Valley. It has resulted in overdose-type situations.”
Fentanyl first hit the streets of Canada in 2014, and has since left a long-lasting scar. Originating in the Vancouver area, it has since spread.
“This issue is not just a Lower Mainland issue, it’s spreading all over,” said Fernie Fire and Rescue Training Officer, Brendan Morgan.
A report from the Ministry of Public Safety and Solicitor General, Office of the Chief Coroner states that there were 211 illicit-drug overdose deaths in 2010, and 914 in 2016. 60 per cent of these were Fentanyl related.
The use of Naloxone as an antidote is nothing new; BC Ambulance Service has been carrying it for thirty years due to the presence of heroin. The difference is that Fentanyl is synthetic opioid pain medication, and many times more potent than heroin.
An overdose of an opioid comes when too much of the drug is taken and it blocks the breathing receptors in the brain, to the point where a person becomes unconscious and in more severe instances, dies.
If necessary in an overdose situation, Naloxone is administered into the muscle, via the thigh or shoulder. One dose can last up to 90 minutes, depending on the individual. First responders are allowed to give up to a maximum of two doses if the overdose requires it.
Naloxone combats the effects of opioids, by assisting in the breathing of the victim, however if a first responder is ventilating the victim properly, the use of Naloxone is unnecessary.
“They made it pretty clear that it’s super important to have the Naloxone, but it’s even more important to get ventilations like bag valve masks, as well as treating them with breathing before,” said Morgan.
In order for first responders to administer Naloxone, a victim must have pinpoint pupils, be unconscious, as well as have a breathing issue, which is defined by less than 10 breaths per minute.
On a regular basis, Fernie Fire and Rescue does not receive many drug-related calls of any kind, and they are thankful for this. However, there are increased instances of cocaine, and various party drugs such as MDMA and Ecstasy being laced with Fentanyl.
“Fernie Fire and Rescue has found it to be quite important now, with the kind of town it is, with the Calgary market and the party atmosphere, we want to get on board and be ready for a situation where we do have an opioid-related issue,” said Morgan.
Morgan has served as training officer for three years, and has been with the department a total of 16 years. There are six career officers plus the chief, as well as 20 auxiliary members. When an auxiliary officer has been with the centre for six months, they are able to receive training as a first responder.
There is always one career (full-time) member on shift, and one career member on call, 24-hours a day. One or two auxiliary members are on pager 56, which is a pager specifically for first responders. Fernie Fire and Rescue will respond as first responders if a code three is announced, which pertains to a lights and sirens emergency.
Time is of the essence during an opioid overdose, which is why Fire and Rescue have been trained to give the antidote if they arrive at the scene before EMS.
“For us as first responders to actually give intermuscular injections, it’s got to be a pretty big crisis,” said Morgan. “Because that’s not something we’d generally do.”
Fentanyl has unofficially arrived in the Elk Valley, and although it has not become a widespread issue yet, emergency crews across the board are ready and prepared to deal with it as best they can.